Preamble
Since the publication of the book Train Aerodynamics – Fundamentals and Applications in 2019, I have published brief annual reviews of published papers in the field of train aerodynamics. Last year, in response to a plethora of poor quality papers, and the increasing use of sophisticated CFD techniques to tackle somewhat trivial problems, I changed the format slightly and presented brief comments on the ten “best” papers published in 2021. This seems to have been a popular format and has attracted almost 400 views in the last year, so I will repeat it this year. The concept of “best” is of course a wholly subjective one, and in reality, I have chosen the papers that follow for a number of reasons – their intrinsic quality, the fact that they address novel issues, or that the subject matter simply interests me. There are no doubt others I could have included. Nine out of the ten come from the Journal of Wind Engineering and Industrial Aerodynamics, which seems to have established its place as the leading journal in this field.
2022 seems to have been the “year of the wind fence” with a number of papers looking at the effectiveness of wind fences of different types and in different locations in protecting trains from cross winds, using both computational and experimental techniques. Although most of these have been competently carried out within their limitations, to choose just one for the following list would have been difficult, and I have thus chosen not to include any. The papers that are presented are arranged in a number of sections that correspond to Chapters in Train Aerodynamics – Fundamentals and Applications – pressure transients (2 papers), pantographs (1), trains in high winds (3), trains in tunnels (3) and emerging issues (1).
Finally, on a personal note, it has now been five years since I retired from the University of Birmingham, and I am very conscious that I am to some degree losing contact with the latest developments in the rail industry. Thus, whilst I will continue to keep an eye on train aerodynamics papers and may well comments on them individually in this blog, this will be my last annual review of the field. Unless of course I change my mind.
Pressure transients
600 km/h moving model rig for high-speed train aerodynamics
A maglev train with a speed of 600 km/h or higher can fill the speed gap between civil aircrafts and wheel rail trains to alleviate the contradiction between the existing transportation demand and actual transport capacity. However, the aerodynamic problems arising due to trains running at a higher speed threaten their safety and fuel efficiency. Therefore, we developed a newly moving model rig with a maximum speed of 680 km/h to evaluate aerodynamic performance of trains, thus determining the range of the aerodynamic design parameters. In the present work, a launch system with a mechanical efficiency of 68.1% was developed, and a structure of brake shoes with front and rear overlapping was designed to increase the friction. Additionally, a device to suppress the pressure disturbances generated by the compressed air, as well as a double track with the function of continuously adjusting the line spacing, were adopted. In repetitive experiments, the time histories of pressure curves for the same measuring point are in good agreement. Meanwhile, the moving model test and full-scale experimental result of maglev trains passing each other in open air are compared, with an error less than 4.6%, proving the repeatability and rationality of the proposed moving model.
This paper is mainly concerned with a description of a new 600 km/h moving model rig at Changsha in China. It is a remarkable piece of equipment, with sophisticated firing and braking systems. The development costs must have been significant. Having worked with moving model rigs in the past, I know that they can be prone to continual minor breakdown and breakages, particularly at high speeds, and it would be nice to know how reliable the new rig is, how many runs can be achieved in a day and so on. From the picture showing the maglev model that was used, there can already be seen to be signs of damage! The experimental results that are shown are not particularly novel, and one wonders if the equivalent results could not have been obtained on lower speed rigs and then scaled by (velocity)2. But nonetheless the authors (all seven of them) are to be congratulated on their efforts
Characteristics of transient pressure in lining cracks induced by high-speed trains.
Rapidly changing pressure waves in the tunnel can aggravate the crack propagation and cause concrete blocks to fall off, posing a threat to trains. Therefore, the influences of aerodynamic pressure on the lining cracks should be considered for high-speed railway tunnels in service. In this paper, the governing equations of air in cracks were derived based on the conservation of mass, momentum, and energy, which was verified by numerical simulations using the software FLUENT. The proposed model was used to analyze the influence of train speed and crack shape on the pressure distribution, peak value and pressure waveform in the crack. Subsequently, the crack tip damage was calculated. The results show that the abrupt change of pressure can amplify the pressure and damage of the crack tip, which can be aggravated by the increase of train speed and crack mouth width.
I found this a really interesting paper that addresses an issue that has not been considered in the past – the amplification of tunnel pressure transients within cracks in the concrete lining of tunnels leading to further damage and crack growth. It is a very neat combination of a theoretical approach informed by CFD work, that leads into a structural damage assessment. Clearly the authors have given considerable thought to the issue and have used the analytical and computational tools at their disposal wisely and intelligently.
Pantographs
Influence of train roof boundary layer on the pantograph aerodynamic uplift: A proposal for a simplified evaluation method
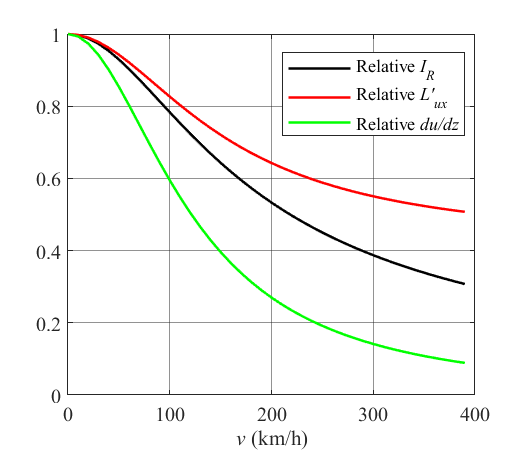
The mean contact force between pantograph collectors and contact wire is affected by the aerodynamic uplift generated by aerodynamic forces acting on pantograph components. For a given pantograph geometry, orientation and working height, aerodynamic forces are strongly influenced by the position of the pantograph along the train roof, since an aerodynamic boundary layer grows along the train. This paper shows the experimental results of aerodynamic uplifts of full-scale pantographs located at four different positions along the roof of a high-speed train and adopts CFD simulations to examine the effect of the boundary layer velocity profile on the measured experimental forces. It is quantitatively demonstrated that the same pantograph located at different positions along the train roof can show relevant differences in the aerodynamic uplift, only due to the different flow characteristics. Moreover, a new simplified methodology is proposed to evaluate the aerodynamic uplifts at different positions of the pantograph along the train. Results of the proposed methodology are validated against full scale experimental results and full CFD simulations exploiting the complete model of the pantograph installed on the train roof.
This paper addresses an issue that has long been ignored – how the varying nature of the boundary layer on the train roof affects the aerodynamic performance of pantographs. In the past the aerodynamic coefficients have been assumed not to vary wherever the pantograph was placed in relation to the train nose. It represents a very elegant combination of large-scale wind tunnel experiments and CFD analysis, exploiting the strength of both methodologies, and leads to a straightforward and practical design methodology.
Trains in high winds
Wind tunnel test on the aerodynamic admittance of a rail vehicle in crosswinds
The aerodynamic admittance of a rail vehicle was investigated by wind tunnel test. Aerodynamic force was measured in the cases of three typical railway structures, including on the flat ground, above an embankment, and on a bridge, under two turbulent flow fields. First of all, three-component aerodynamic coefficients of the vehicle on each structure were obtained under uniform flow with respect to three wind attack angles and four wind direction angles. Secondly, the aerodynamic forces on the vehicle and the corresponding wind speed were evaluated to establish an aerodynamic admittance function of the vehicle. The aerodynamic admittance of the rail vehicle approximated a constant value in the low-frequency domain, but decreased with the reduced frequency increasing. The effects of the different reduced frequencies on the drag are greater than the lift admittance of the vehicle, while moment admittance stays steady-state. Finally, in order to reflect the unsteady characteristics of the buffeting force on the vehicle, the aerodynamic admittance functions of the vehicle were fitted to the expression of the frequency response function of a mass-spring-damping system, which was then verified. Furthermore, the effects of flat terrain and mountainous terrain were investigated, revealing that the influence of turbulence intensity on aerodynamic admittance is significant.
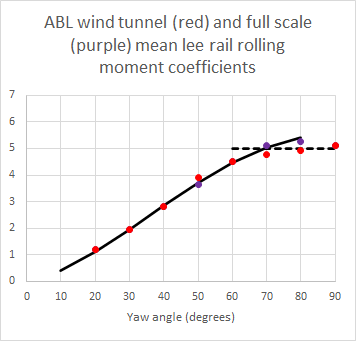
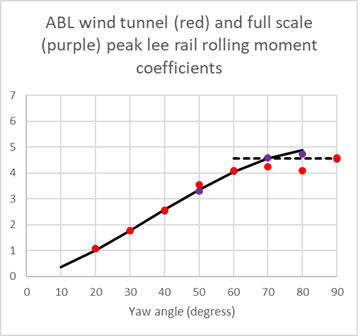
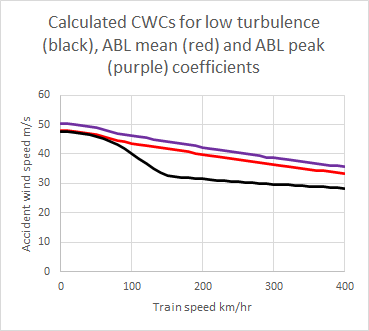
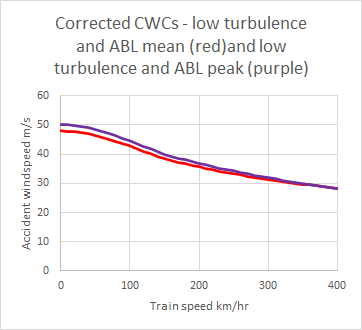
This experimental paper is the companion of a more theoretical one that was also published in 2022. This theoretical approach to describing aerodynamic admittances is based on work that I carried out in 2010, and it is good to see it much more fully investigated experimentally than myself and my co-workers were able to achieve at the time, with high quality aerodynamic admittance data being obtained for a range of turbulence simulations, and infrastructure and train geometries. There is more work to do however, in investigating just how important the concept of aerodynamic admittance actually is in train overturning calculations and how does its use affect the magnitude of the crosswind characteristics or CWCs (plots of accident wind speed against vehicle speed). The limited work myself and colleagues carried out on this a decade ago as we were developing a simple analytical framework for CWCs would suggest the effect is small, but it would be good to quantify this, and the results outlined in this paper would enable this to be done.
Impact of the train-track-bridge system characteristics in the runnability of high-speed trains against crosswinds – Part I: Running safety
This paper studies the influence of different factors related to the structure-track-vehicle coupling system in the train’s stability against crosswinds, namely the bridge lateral behaviour, the track condition and the train type. With respect to the former, a parametrization of an existing long viaduct with high piers has been carried out to simulate different lateral flexibilities. The study concluded that the bridge’s lateral behaviour has a negligible impact in wind-induced derailments. Dynamic analyses considering four scenarios of track condition, ranging from ideal to poorer condition, but still within the limits stipulated by the codes, have also been carried out, leading to the conclusion that the track irregularities influence the running safety mainly on the higher train speed levels. This is due to the fact that the Nadal and Prud’homme indexes strongly depend on the wheel-rail lateral impacts, which become more pronounced for higher speeds and under poorer track conditions. Finally, four different trains have been adopted in the study to cover a wide range of vehicles. The results proved the importance of carefully considering the trains used in the analysis, since the train’s weight may vary significantly, leading to considerable different results in terms of vehicle’s stability against lateral winds.
This is the first of a two-part paper that considers the effect of various system characteristics on train behaviour in cross winds. This paper considers the safety issue, whilst its companion considers passenger comfort issues. The analysis uses simulations of wind fields, with a sophisticated MDOF train dynamic model and looks at the effect of bridge flexibility, track roughness and train type. With regard to the former, the effects on the calculated CWCs is small. Whilst this calculation is for a concrete viaduct, the results must cast considerable doubt on the analysis of a plethora of recent papers that have considered the movement of trains over bridge of different types, using highly complex methodology to describe bridge vibrations – was such complexity really required? The effect of track roughness on CWCS was shown to be somewhat more significant and is an issue that perhaps needs to be taken into account in any future work in my view. Finally, and intriguingly, the authors show that in some instances the Prud’homme derailment criterion is critical rather than the train stability criterion and suggest that this effect ought to be taken into account in the development of CWCS. This is a significant paper, and, with seven authors, shares the prize for most contributors in this selection. They are all to be applauded!
Numerical study of tornado-induced unsteady crosswind response of railway vehicle using multibody dynamic simulations.
The tornado-induced unsteady crosswind responses of railway vehicles are investigated by using multibody dynamic simulations. Firstly, a tornado-induced aerodynamic force model is proposed by using the equivalent wind force method and the quasi-steady theory and validated by the experimental data. The Uetsu line railway accident caused by tornado winds on December 25, 2005 is then investigated by the proposed tornado-induced aerodynamic force model and the multi-body dynamic simulation. The predicted accident scenes show favorably agreement with those obtained from the accident survey when the maximum tangential velocity of tornado is around 41 m/s and the core radius is 30m. Finally, the dynamic amplification factor (DAF) for railway vehicles in tornado winds is systematically studied and it increases as the passing time decreases. It is found that the DAF can be effectively suppressed as the damping parameters increase while it decreases slightly as the natural frequency increases. A simple method to predict the DAF is also proposed based on simulation results.
This paper addresses an ongoing issue in the study of the effect of cross winds on trains – is the quasi-steady methodology adequate or are more complex models required – this time in the context of vary rapidly varying tornado loading. In the analysis the use of the discontinuous Rankine model (without radial inflow) and Burgers Rott model (which was used way outside its low Reynolds number region of applicability) somewhat limits the adequacy of the analysis, but probably not in a very significant way. The modelling is calibrated using a low speed moving model experiment. The use of the dynamic model enables significant details of the overturning process to be revealed, and shows that for rapid changes in flow velocity, there are significant overshoots in train forces from the quasi-steady values. I do wonder however, in view of the fact that tornado wind field modelling is a very uncertain procedure (and likely to remain as such) whether the complexity of the use of dynamic models is actually justified. The jury is still out on this issue I think.
Trains in tunnels
Micro-pressure wave radiation from tunnel portals in deep cuttings
The reflection and radiation of steep-fronted wavefronts at a tunnel exit to a deep cutting is studied and contrasted with the more usual case of radiation from over-ground portals. A well-known difference between radiation in odd and even dimensions is shown to have a significant influence on reflected wavefronts, notably causing increased distortion that complicates analyses, but that can have practical advantages when rapid changes are undesirable. Likewise, micro-pressure waves radiating from the portal into a cutting are shown to exhibit strong dispersion that does not occur in the corresponding radiation into an open terrain. In the latter case, formulae that represent the behaviour of monopoles and dipoles are commonly used to estimate conditions beyond tunnel portals, but no such simple formula exists (or is even possible) for cylindrical radiation that is characteristic of MPWs in cuttings. An important outcome of the paper is the development of an approximate relationship that predicts the maximum amplitudes of these MPWs with an accuracy that should be acceptable in engineering design, at least for initial purposes. The formula shows that peak pressure amplitudes decay much more slowly than those from an overground portal, namely varying approximately as r 0.5 compared with r 1, where r denotes the distance from the portal.
This paper describes a thoughtful, analytical study that addresses the effects of deep cuttings at the exit of tunnels on the reflected and transmitted pressure waves. It is shown that the reflected waves take longer to develop and are more spread out than with a tunnel outlet on level ground and that the radiating pressure wave (the MPVs) decay much less rapidly. The paper gets to the heart of the basic assumptions underlying tunnel pressure wave analysis and brings to light issues that users of commercial software need to be very aware of.
Experimental study on transient pressure induced by high-speed train passing through an underground station with adjoining tunnels
Transient pressure variations on train and platform screen door (PSD) surfaces when a high-speed train passed through an underground station and adjoining tunnel were studied using a moving model test device based on the eight-car formation train model. The propagation characteristics of the pressure wave that was induced when the train passed through the station and tunnel at a high speed were discussed, and the effects of the train speed and station ventilation shaft position on the surface pressure distribution of the train and PSDs were analyzed and compared. The results showed that the pressure fluctuation law is different for the train and PSD surfaces, and the peak pressure increases significantly with an increase in the train speed. Ventilation shafts changed the pressure waveform on the surface of the train and PSDs and greatly reduced the peak pressure. A single shaft at the rear end of the platform and a double shaft at the station had the most significant effect on relieving transient pressure on the surface of the train and PSDs, respectively. Compared with the case with no shaft, these two shafts reduced the maximum amplitude pressure variation of the train and PSD surfaces by 46.3% and 67.4%, respectively.
This paper describes a nicely set up and carried out series of experiments using a moving model rig. The situation that is considered (an underground station in a high-speed tunnel network) is quite generic and could form a useful test case for airflow calculation methods. The effect of air shafts on reducing pressures is very clear. It would have been nice to see more variations of air shaft geometry in the experimental programme, but the authors probably felt they had more than enough to do.
Field test for micro-pressure wave reduction measurement by area optimization of windows of tunnel hoods.
The air compression of a high-speed train entering a tunnel results in micro-pressure waves (MPWs), which can cause environmental problems. To mitigate MPWs, tunnel hoods with discrete windows are installed at the tunnel entrances. By properly adjusting the window conditions, the efficiency of the tunnel hood in mitigating MPWs can be enhanced. Per Japanese convention, window conditions are optimized by changing the opening/closing pattern in the longitudinal direction (pattern optimization). The optimization pattern of the windows is fundamentally different if there is a change in the train speed, train nose length, the relative position between the train and the windows, or the train nose shape. Therefore, for extremely long tunnel hoods, the optimal state of the windows is almost impossible to detect numerically or experimentally using pattern optimization. In this study, we realized a rapid and simple optimization of the windows of the tunnel hood (i.e., area optimization) for mitigation of MPWs by field measurements. The result demonstrated that the area optimization considerably helps in mitigating the MPWs, despite the simplicity of the procedures.
To reduce MPW magnitudes, the initial gradient of the pressure waves caused by train entry into the tunnel need to be minimised (since these steepen along the tunnel, with steeper waves producing stronger radiated MPWs at the outlet). One way of doing this is to design a variable area entrance hood, with openings along the side so that the pressure wave builds up gradually. The optimisation of these openings has in the past been somewhat hit and miss, and it difficult to know what is the optimal configuration. This paper describes a simple optimization methodology and presents a series of quite ambitious full-scale experiments to validate this methodology. The final result is a very simple but effective arrangement of openings which represents the best that can be achieved.
Emerging issues
Diffusion characteristics and risk assessment of respiratory pollutants in high-speed train carriages
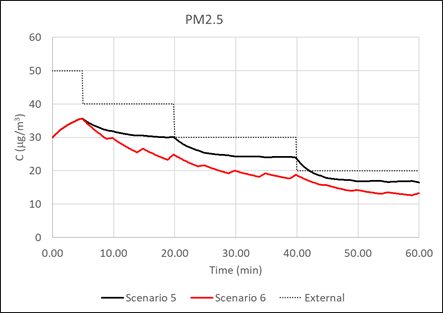
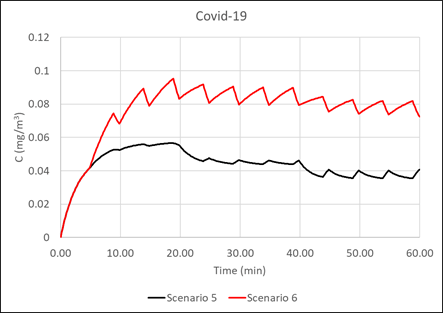
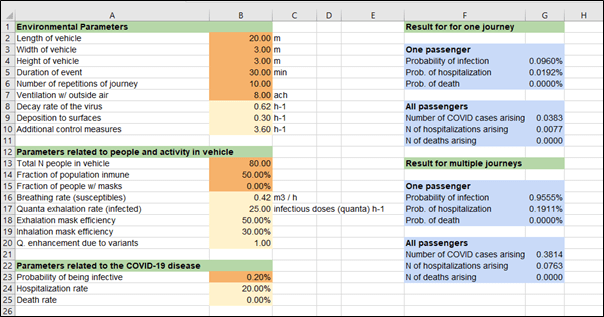
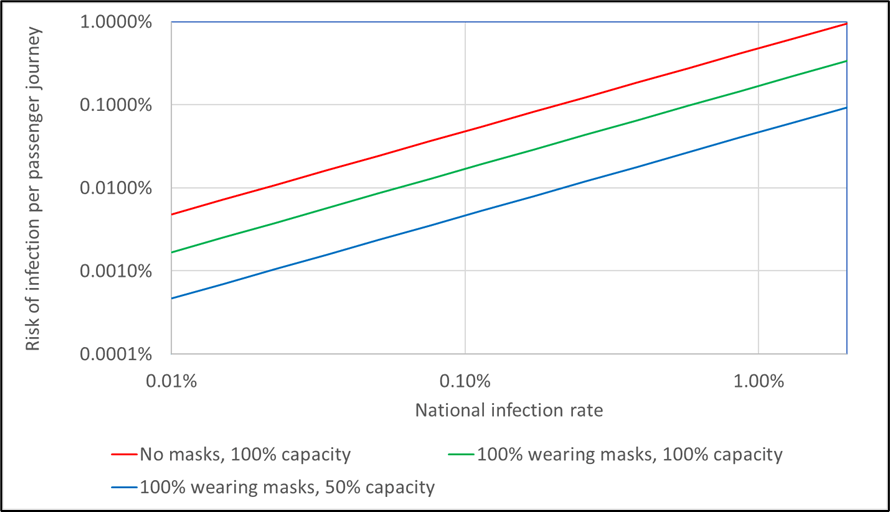
Due to the density of people in the cabins of high-speed trains, and the development of the transportation network, respiratory diseases are easily transmitted and spread to various cities. In the context of the epidemic, studying the diffusion characteristics of respiratory pollutants in the cabin and the distribution of passengers is of great significance to the protection of the health of passengers. Based on the theory of computational fluid dynamics (CFD), a high-speed train cabin model with a complete air supply duct is established. For both summer and winter conditions, the characteristics of the flow field and temperature field in the cabin, under full load capacity, and the diffusion characteristics of respiratory pollutants under half load capacity are studied. Taking COVID-19 as an example, the probability of passengers being infected was evaluated. Furthermore, research on the layout of this type of cabin was carried out. The results show that it is not favorable to exhaust air at both ends, as this is likely to cause large-area diffusion of pollutants. The air barrier formed in the aisle can assist the ventilation system, which can prevent pollutants from spreading from one side to the other. Along the length of the train, the respiratory pollutants of passengers almost always spread only forward or backward. Moreover, when the distance between passengers and the infector exceeds one row, the probability of being infected does not decrease significantly. In order to reduce the probability of cross infection, and take into account the passenger efficiency of the railway, passengers in the same row should be separated from each other, and it is best to ride on both sides of the aisle. In the same column, passengers only need to be separated by one row, and it is not recommended to use the middle of the carriage. The number of passengers in the front and back half of the cabin should also be roughly the same.
This is an interesting and important paper, arising of course out of the recent pandemic. Through the use of reasonably straightforward CFD methodology, the spread of pathogen from any point within a railway carriage to any other point can be calculated, and from this the probability of infection can be ascertained. This methodology may have widespread future use and can be used to inform passenger loading configurations with to minimise infection probabilities. The calculations were restricted to likely infection from an infected passenger in a small number of locations. There is no reason why the number of locations should not equal the number of possible passenger conditions and a matrix produced on of infection in seat i due to an infected individual in seat j, which would enable a fuller picture of infection rates to be developed.